Key Takeaways
- Gold Standard: PSG is the most accurate way to diagnose complex sleep disorders.
- Comprehensive: It tracks brain waves, heart rate, breathing, and movement simultaneously.
- In-Lab Experience: Typically involves an overnight stay in a controlled clinic environment.
- Beyond Apnea: Essential for diagnosing narcolepsy, parasomnias, and central sleep apnea.
Why a Basic Home Test Isn't Always Enough
You might have seen ads for home sleep apnea tests that only track a few things, like your oxygen levels or airflow. While convenient, these are essentially "lite" versions of a real study. A home test might tell you that you stop breathing, but it can't tell you why or how it affects your sleep stages.
A full polysomnography study monitors at least seven different physiological markers. This allows doctors to see the transition between NREM (Non-Rapid Eye Movement) and REM (Rapid Eye Movement) sleep. If you have narcolepsy, for instance, you might skip the line and jump straight into REM sleep. A home test would miss that entirely, but a PSG catches it in real-time.
The Tech: What Exactly Are They Measuring?
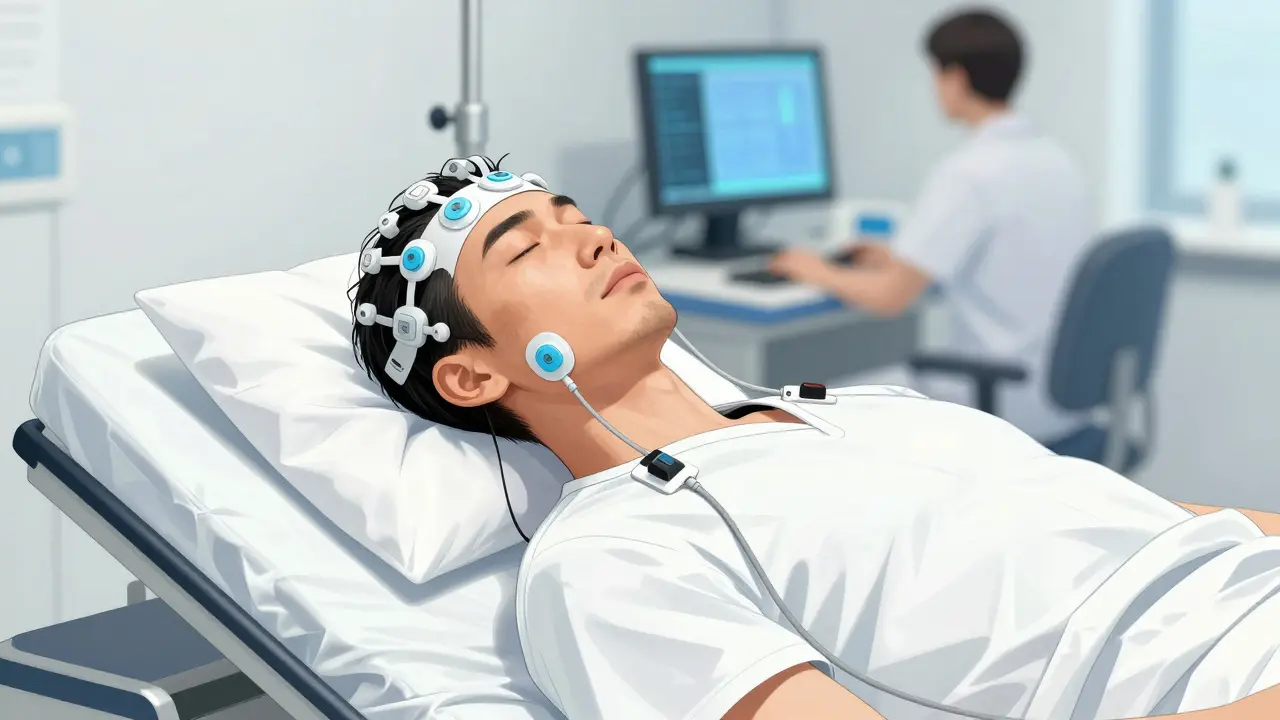
Walking into a sleep lab can feel like walking into a sci-fi movie. You'll see a variety of sensors and wires, but each one has a specific job. To get a clear picture of your health, technicians track the following:
- Brain Activity: Using an Electroencephalogram (EEG), electrodes on your scalp track brain waves to determine which stage of sleep you are in.
- Eye & Muscle Movement: An Electrooculogram (EOG) tracks eye movements (crucial for REM detection), while an Electromyogram (EMG) monitors muscle tone in your chin and legs to spot abnormal movements.
- Heart & Breathing: An Electrocardiogram (ECG) checks your heart rhythm, while belts around your chest and nasal sensors monitor your airflow and breathing effort.
- Oxygen & Position: Pulse oximetry clips track blood oxygen levels, and sensors on your body tell the doctor if your apnea only happens when you sleep on your back.
| Feature | Polysomnography (In-Lab) | Home Sleep Test (HSAT) |
|---|---|---|
| Parameters Tracked | 7 to 16 (Full Suite) | 3 to 4 (Basic) |
| Sleep Staging (REM/NREM) | Yes (EEG provided) | No |
| Failure Rate | Low (2-5%) | Higher (15-20%) |
| Complexity of Diagnosis | High (Narcolepsy, PLMD, etc.) | Low (Mainly Obstructive Sleep Apnea) |
| Environment | Controlled Clinical Setting | Patient's Own Bed |
The Experience: Your First Night in the Lab
If you're nervous about the wires, you aren't alone. Most people worry that they won't be able to sleep in a strange room with 22 sensors attached to them. In reality, about 85% of patients complete the study successfully. The rooms are usually kept between 68-72°F to help you drift off, and the staff are experts at making you feel comfortable.
The process starts with a 30-45 minute setup. You'll arrive a couple of hours before your usual bedtime. A registered sleep technologist will place the electrodes and sensors. While you're in your private room, the technologist is monitoring everything from an adjacent room. If a sensor peels off or you need something, they can communicate with you immediately.
Pro tip: To get the best results, avoid caffeine after noon on the day of your test and stick to your normal wake-up time for a few days leading up to the appointment. This ensures the data reflects your actual daily struggle, not a fluke caused by an afternoon espresso.
Decoding the Results: What Does the Doctor Look For?
After you wake up and the sensors come off, the real work begins. Your night of sleep generates over 1,000 pages of raw data. A board-certified sleep physician spends several hours analyzing this data to find patterns. They aren't just looking for "stopped breathing"; they are looking for the type of interruption.
For example, the PSG can distinguish between Obstructive Sleep Apnea and Central Sleep Apnea. In obstructive apnea, the brain is trying to breathe, but the airway is blocked. In central apnea, the brain simply forgets to tell the muscles to breathe. This distinction is vital because the treatments for each are very different.
They also look for "micro-arousals." These are brief awakenings that you don't even remember but that kick you out of deep sleep and back into light sleep. This is why you can sleep for eight hours but still wake up feeling like you've been hit by a truck.

Specialized Versions: Split-Nights and Titrations
Sometimes, a standard diagnostic test is just the first step. If a doctor is very confident you have sleep apnea, they might suggest a "split-night" study. In the first half of the night, they diagnose the condition. If the data shows severe apnea early on, they spend the second half of the night doing a CPAP Titration. This means they introduce a Continuous Positive Airway Pressure machine to find the exact pressure setting that keeps your airway open.
This saves you a second trip to the clinic. Instead of coming back another night to find your settings, you leave the lab with both a diagnosis and a prescription for the exact pressure your body needs.
Is polysomnography painful?
No, it is completely non-invasive. The sensors are adhered to your skin with medical tape or lightly strapped to your body. The only discomfort is usually the feeling of being "wired up" and the challenge of sleeping in an unfamiliar environment.
How long does it take to get the results?
Because a single night produces a massive amount of data, it typically takes a few days to a couple of weeks for a physician to review the recordings and generate a final diagnostic report.
Will insurance cover a sleep study?
Most insurance providers, including Medicare, cover PSG if you meet specific clinical criteria, such as documented daytime sleepiness, snoring, or witnessed apneas. However, many private insurers require prior authorization before the test is performed.
What happens if I can't fall asleep during the test?
It's common to have some trouble sleeping the first night. Sleep technologists are trained to help you relax. If you truly cannot sleep enough for the data to be valid, the clinic may suggest a second night to let you acclimate to the environment.
Can a PSG diagnose narcolepsy?
Yes. Because PSG monitors sleep staging via EEG, it can detect if a patient enters REM sleep too quickly. This is often followed by a Multiple Sleep Latency Test (MSLT) the next day to confirm the diagnosis by measuring how quickly you fall asleep during scheduled naps.
Next Steps After Your Study
Once you have your results, the path forward depends on the findings. If the diagnosis is Obstructive Sleep Apnea, the next step is usually starting CPAP therapy or exploring oral appliances. If the study shows Periodic Limb Movement Disorder (PLMD), your doctor might look into medication or lifestyle changes.
If your results were "normal" but you still feel exhausted, don't give up. Ask your doctor about a follow-up MSLT or an evaluation for other conditions like restless legs syndrome or insomnia. The PSG is a powerful tool, but it's one piece of a larger puzzle in managing your health.

Had a PSG last year and it was a total game changer for my energy levels. The weirdest part is definitely the sticky paste they use for the EEG electrodes, but it's a small price to pay for actually knowing why you're exhausted. For anyone nervous about the 'wired up' feeling, just remember that the techs are super chill and they've seen it all. Once you get your CPAP settings dialed in from a titration study, you'll wonder how you ever survived without it. It's honestly like flipping a switch in your brain to actually feel awake for the first time in years.